Heart Rhythm Services
Watchman LAAC Implant
The WATCHMAN device is a parachute-shaped self-expanding device permanently implanted in the LAA sealing it off. It prevents blood clots in the LAA from entering the bloodstream. It is made of materials that are common to many medical devices, is about the size of a quarter, and it cannot be seen outside the body.
How is the WATCHMAN device implanted?
The WATCHMAN Implant is typically performed while you are asleep. Your doctor will guide the WATCHMAN device into your heart through a flexible tube (catheter) inserted through a vein in your upper leg. Once the position is confirmed, your doctor will release the implant to leave it permanently in the heart. The implant does not require open heart surgery. After 6 weeks, you may be able to stop taking your blood thinner.
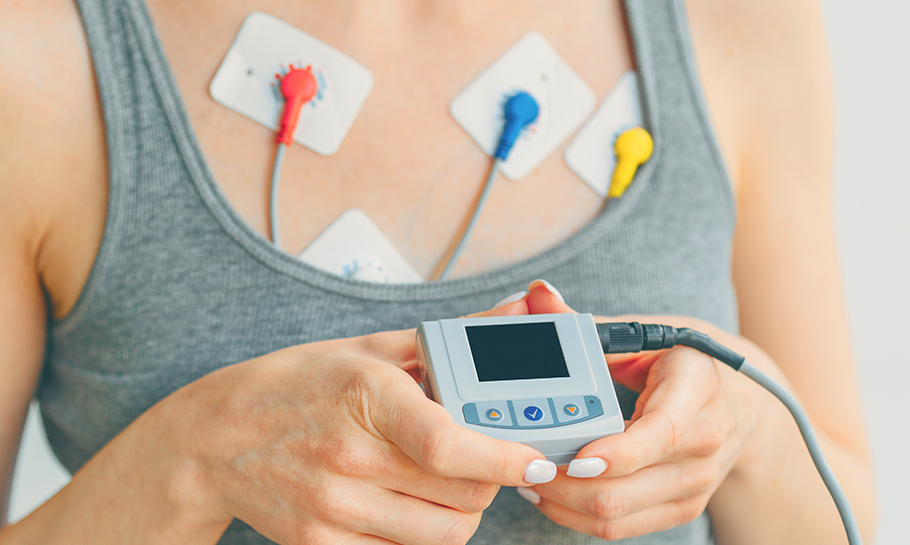
Electrophysiology Procedures - Understanding Your Heart's Activity
An electrophysiology (EP) study is a test that checks how your heart's electrical system is working. This helps diagnose any abnormal heartbeats or arrhythmias you might have. During the test, we use catheters (thin tubes) with wire electrodes to measure the electrical activity of your heart. These catheters are gently inserted through blood vessels and into your heart.
Ablation - Treating Atrial Fibrillation
Ablation is a procedure used to treat atrial fibrillation, a condition where your heart beats irregularly. We use small burns or freezing to create some scarring on the inside of your heart. This helps break up the electrical signals causing the irregular heartbeat. By doing this, we help your heart maintain a normal rhythm, making you feel better.
Pacemaker - Regulating Slow Heartbeats
If you have slow electrical problems with your heart, a pacemaker can help. It's a small electronic device that we implant in your chest, usually just below the collarbone. The pacemaker helps regulate your heartbeat, ensuring it doesn't slow down to a dangerously low rate. With a pacemaker, your heart can beat at a steady and healthy pace.
Biventricular Pacemaker - A Newer Solution for Heart Failure
For specific types of heart failure, a newer type of pacemaker called a biventricular pacemaker is used. In heart failure, sometimes the two ventricles (the lower chambers of the heart) don't pump normally. This is called ventricular dyssynchrony, and it reduces the amount of blood pumped by the heart.
The biventricular pacemaker paces both ventricles at the same time, helping the heart pump more efficiently. This treatment is known as cardiac resynchronization therapy (CRT), and it can greatly improve your heart's function, making you feel better and improving your quality of life.